Which Are The Major Causes Of Posterior Tibial Tendon Dysfunction (PTTD) ?
Overview
Noticed that your foot is getting flatter and more painful? Do you have difficulty walking or performing exercise activity without leg and arch pain? Have you heard the term "fallen arches"? All of these things refer to a condition known as posterior tibial tendon dysfunction. This is an inflammation and overuse syndrome of one of the long tendons that pass from the leg around the inside of the ankle and attaches to the inside arch of the foot. The posterior tibial tendon?s job is to help support the arch and allow for more efficient gait. 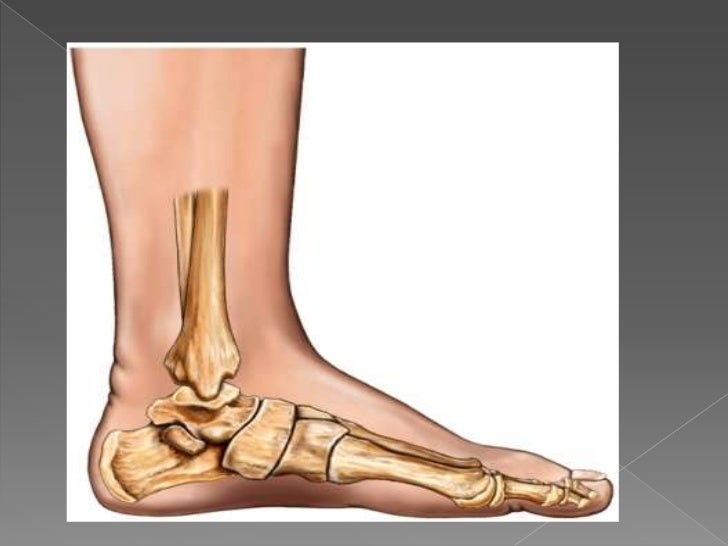
Causes
Damage to the posterior tendon from overuse is the most common cause for adult acquired flatfoot. Running, walking, hiking, and climbing stairs are activities that add stress to this tendon, and this overuse can lead to damage. Obesity, previous ankle surgery or trauma, diabetes (Charcot foot), and rheumatoid arthritis are other common risk factors.
Symptoms
Some symptoms of adult acquired flat foot are pain along the inside of the foot and ankle, pain that increases with activity, and difficulty walking for long periods of time. You may experience difficulty standing, pain on the outside of the ankle, and bony bumps on the top of the foot and inside the foot. You may also have numbness and tingling of the feet and toes (may result from large bone spurs putting pressure on nerves), swelling, a large bump on the sole of the foot and/or an ulcer (in diabetic patients). Diabetic patients should wear a properly fitting diabetic shoe wear to prevent these complications from happening.
Diagnosis
Observation by a skilled foot clinician and a hands-on evaluation of the foot and ankle is the most accurate diagnostic technique. Your Dallas foot doctor may have you do a walking examination (the most reliable way to check for the deformity). During walking, the affected foot appears more pronated and deformed. Your podiatrist may do muscle testing to look for strength deficiencies. During a single foot raise test, the foot doctor will ask you to rise up on the tip of your toes while keeping your unaffected foot off the ground. If your posterior tendon has been attenuated or ruptured, you will be unable to lift your heel off the floor. In less severe cases, it is possible to rise onto your toes, but your heel will not invert normally. X-rays are not always helpful as a diagnostic tool for Adult Flatfoot because both feet will generally demonstrate a deformity. MRI (magnetic resonance imaging) may show tendon injury and inflammation, but can?t always be relied on for a complete diagnosis. In most cases, a MRI is not necessary to diagnose a posterior tibial tendon injury. An ultrasound may also be used to confirm the deformity, but is usually not required for an initial diagnosis.
Non surgical Treatment
Stage one deformities usually respond to conservative or non-surgical therapy such as anti-inflammatory medication, casting, functional orthotics or a foot ankle orthosis called a Richie Brace. If these modalities are unsuccessful surgery is warranted. 
Surgical Treatment
When conservative care fails to control symptoms and/or deformity, then surgery may be needed. The goal of surgical treatment is to obtain good alignment while keeping the foot and ankle as flexible as possible. The most common procedures used with this condition include arthrodesis (fusion), osteotomy (cutting out a wedge-shaped piece of bone), and lateral column lengthening. Lateral column lengthening involves the use of a bone graft at the calcaneocuboid joint. This procedure helps restore the medial longitudinal arch (arch along the inside of the foot). A torn tendon or spring ligament will be repaired or reconstructed. Other surgical options include tendon shortening or lengthening. Or the surgeon may move one or more tendons. This procedure is called a tendon transfer. Tendon transfer uses another tendon to help the posterior tibial tendon function more effectively. A tendon transfer is designed to change the force and angle of pull on the bones of the arch. It's not clear yet from research evidence which surgical procedure works best for this condition. A combination of surgical treatments may be needed. It may depend on your age, type and severity of deformity and symptoms, and your desired level of daily activity.
Torn Achilles Tendon Symptoms
 The Achilles tendon attaches the calf muscle to the heel bone. Jumping, climbing and strenuous exercise can strain the tendon and calf muscle, which can cause the type of inflammation known as tendinitis. This injury can be mild enough that it can be treated by over-the-counter medications or so severe that it must be repaired surgically. Chronic tendinitis can cause microscopic tears in the muscle which can weaken the tendon and increase the risk for tear or rupture. Symptoms usually include pain and swelling near the ankle. Pain may lead to weakness in the area that increases with walking and running. Stiffness in the tendon may be worse in the morning.
The Achilles tendon attaches the calf muscle to the heel bone. Jumping, climbing and strenuous exercise can strain the tendon and calf muscle, which can cause the type of inflammation known as tendinitis. This injury can be mild enough that it can be treated by over-the-counter medications or so severe that it must be repaired surgically. Chronic tendinitis can cause microscopic tears in the muscle which can weaken the tendon and increase the risk for tear or rupture. Symptoms usually include pain and swelling near the ankle. Pain may lead to weakness in the area that increases with walking and running. Stiffness in the tendon may be worse in the morning.
Causes
Tight or tired calf muscles, which transfer too much of the force associated with running onto the Achilles tendon. Not stretching the calves properly or a rapid increase in intensity and frequency of sport training can make calf muscles fatigued. Activities which place a lot of stress on the achilles tendon, such as hill running and sprint training, can also cause Achilles Tendinitis. Runners who overpronate (roll too far inward on their feet during impact) are most susceptible to Achilles Tendinitis. Runners with flat feet are susceptible to Achilles Tendinitis because flat feet cause a 'wringing out' effect on the achilles tendon during running. High arched feet usually absorb less shock from the impact of running so that shock is transferred to the Achilles tendon. Use of inappropriate footwear when playing sport or running e.g., sandals, can also put an extra load on the Achilles tendon. Shoes are now available that have been designed for individual sports and provide cushioning to absorb the shock of impact and support for the foot during forceful movements. Training on hard surfaces e.g., concrete, also increases the risk of Achilles Tendinitis. Landing heavily or continuously on a hard surface can send a shock through the body which is partly absorbed by the Achilles tendon. A soft surface like grass turf helps to lessen the shock of the impact by absorbing some of the force of the feet landing heavily on the ground after a jump or during a running motion.
Symptoms
Achilles tendonitis is an injury that occurs when your Achilles tendon -- the large band of tissues connecting the muscles in the back of your lower leg to your heel bone -- becomes inflamed or irritated. The signs and symptoms of Achilles tendonitis often develop gradually. You'll feel pain and stiffness in your Achilles, especially when you first get out of bed. The pain lessens as you warm up, and may even disappear as you continue running. Once you stop, the pain returns and may feel even worse. You may also notice a crackling or creaking sound when you touch or move your Achilles tendon.
Diagnosis
If you think you might have Achilles tendonitis, check in with your doctor before it gets any worse. Your doc will ask about the activities you've been doing and will examine your leg, foot, ankle, and knee for range of motion. If your pain is more severe, the doctor may also make sure you haven't ruptured (torn) your Achilles tendon. To check this, the doc might have you lie face down and bend your knee while he or she presses on your calf muscles to see if your foot flexes. Any flexing of the foot means the tendon is at least partly intact. It's possible that the doctor might also order an X-ray or MRI scan of your foot and leg to check for fractures, partial tears of the tendon, or signs of a condition that might get worse. Foot and ankle pain also might be a sign of other overuse injuries that can cause foot and heel pain, like plantar fasciitis and Sever's disease. If you also have any problems like these, they also need to be treated.
Nonsurgical Treatment
Treatment options might include anti-inflammatory medication such as ibuprofen which might help with acute achilles inflammation and pain but has not been proven to be beneficial long term and may even inhibit healing. If the injury is severe then a plaster cast might be applied to immobilize the tendon. Use of electrotherapy such as ultrasound treatment, laser therapy and extracorporeal shock wave therapy (ESWT) may be beneficial in reducing pain and encouraging healing. Applying sports massage techniques can mobilze the tissues or the tendon itself and help stretch the calf muscles. Some might give a steroid injection however an injection directly into the tendon is not recommended. Some specialists believe this can increase the risk of a total rupture of the tendon in future. One of the most effective forms of treatment for achilles tendonitis is a full rehabilitation program consisting of eccentric strengthening exercises. There is now considerable evidence suggesting the effectiveness of slow eccentric rehabilitation exercises for curing achilles tendon pain.
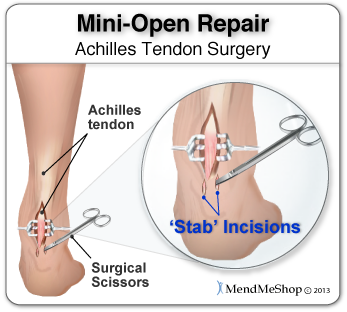
Surgical Treatment
Surgery is an option of last resort. However, if friction between the tendon and its covering sheath makes the sheath thick and fibrous, surgery to remove the fibrous tissue and repair any tears may be the best treatment option.
Prevention
Regardless of whether the Achilles injury is insertional or non-insertional, a great method for lessening stress on the Achilles tendon is flexor digitorum longus exercises. This muscle, which originates along the back of the leg and attaches to the tips of the toes, lies deep to the Achilles. It works synergistically with the soleus muscle to decelerate the forward motion of the leg before the heel leaves the ground during propulsion. This significantly lessens strain on the Achilles tendon as it decelerates elongation of the tendon. Many foot surgeons are aware of the connection between flexor digitorum longus and the Achilles tendon-surgical lengthening of the Achilles (which is done to treat certain congenital problems) almost always results in developing hammer toes as flexor digitorum longus attempts to do the job of the recently lengthened tendon. Finally, avoid having cortisone injected into either the bursa or tendon-doing so weakens the tendon as it shifts production of collagen from type one to type three. In a recent study published in the Journal of Bone Joint Surgery(9), cortisone was shown to lower the stress necessary to rupture the Achilles tendon, and was particularly dangerous when done on both sides, as it produced a systemic effect that further weakened the tendon.
Pes Planus Explained

Flat feet are a usually painless condition where the arches on the inside of your feet are completely collapsed arches so that the entire sole of your feet touch the floor when standing. Flat feet can develop after an injury to the foot, such as a ligament, tendon or muscle tear, or as a result of arthritis or they may develop because the condition runs in the family. People with flat feet often complain of their feet rolling inwards when walking or a feeling of their foot collapsing.
Causes
Most commonly fallen arches in adulthood can arise due to Posterior Tibial Tendon Dysfunction (PTTD). The posterior tibial tendon plays a pivotal role in holding up the arch of the foot, damage to this tendon results in the arch collapsing. Another cause of acquired flat feet in adulthood may be due to Rheumatoid arthritis as this disease attacks the bone, cartilage and ligaments in the foot causing it to change shape and flatten. Injury to the ligament, fracture and/or dislocation of the bones in the mid foot can all lead to a flat foot deformity. Adult acquired flat fleet can also arise in people who have diabetes or a neurological condition which limits normal feeling in the foot, the muscles in feet switch off, the tendons and ligaments weaken, and the arch eventually collapses.
Symptoms
The primary symptom of flatfeet is the absence of an arch upon standing. Additional signs of flatfeet include the following. Foot pain. Pain or weakness in the lower legs. Pain or swelling on the inside of the ankle. Uneven shoe wear. While most cases of flatfeet do not cause problems, complications can sometimes occur. Complications include the following, bunions and calluses, inability to walk or run normally, inflammation and pain in the bottom of the foot (plantar fasciitis), tendonitis in the Achilles heel and other ligaments, pain in the ankles, knees, and hips due to improper alignment, shin splints, stress fractures in the lower legs.
Diagnosis
Your doctor examines your feet to determine two things, whether you have flat feet and the cause or causes. An exam may include the following steps, Checking your health history for evidence of illnesses or injuries that could be linked to flat feet or fallen arches, Looking at the soles of your shoes for unusual wear patterns, Observing the feet and legs as you stand and do simple movements, such as raising up on your toes, Testing the strength of muscles and tendons, including other tendons in the feet and legs, such as the Achilles tendon or the posterior tibial tendon, Taking X-rays or an MRI of your feet.
Non Surgical Treatment
Flexible flat feet that are painless do not require treatment. If you have pain due to flexible flat feet, an orthotic (arch-supporting insert in the shoe) can bring relief. With the increased interest in running, many shoe stores carry shoes for normal feet and pronated feet. The shoes designed for pronated feet make long distance running easier and less tiring because they correct for the abnormality. Rigid or painful flat feet require evaluation by a health care provider. The treatment depends on the cause of the flat feet. For tarsal coalition, treatment starts with rest and possibly a cast. If this fails to improve the pain, surgery may be necessary. For problems with the posterior tibial tendon, treatment may start with rest, anti-inflammatory medications, and shoe inserts or ankle braces. In more advanced cases, surgery may be needed to clean or repair the tendon, or fuse some of the joints of the foot into a corrected position. Flat feet in older adults can be treated with pain relievers, orthotics, and sometimes surgery.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
Coping With Pain In The Arch
Arch pain (medically known as plantar pain) is a broad term many people use to describe pain in their muscles, tendons, ligaments, bones, or nerves. All these components are connected to the bottom of the foot; therefore, damage to any one of these can cause pain on the bottom of the foot. This pain may only last for short time, but can progressively worsen if untreated. Most people who suffer from this pain are between the ages of 30 and 80, but many younger athletes are also susceptible, particularly those who participate in high-impact sports.

Causes
The most common cause of arch pain is plantar fasciitis. Plantar fasciitis is inflammation of the fibrous band of tissue that connects the heel to the toes. Sufferers of plantar fasciitis typically feel pain early in the morning when they first get out of bed. Another common cause of arch pain is fallen arches or flat feet. Fallen arches result in the sole of the foot becoming flat so that the entire sole of the foot touches the ground. Fallen arches can lead to pain in the ankles, knees, feet, and even in the legs. While fallen arches are often inherited, for some it develops as a result of wear and tear on your feet. Wearing shoes without proper metatarsal support, or arch support, can overstretch the tendon that supports the arch causing the arch to flatten out.
Symptoms
Many people have no symptoms, and the condition is discovered only by chance when an X-ray of the foot is obtained for some other problem. When symptoms occur, there is usually foot pain that begins at the outside rear of the foot. The pain tends to spread upward to the outer ankle and to the outside portion of the lower leg. Symptoms usually start during a child's teenage years and are aggravated by playing sports or walking on uneven ground. In some cases, the condition is discovered when a child is evaluated for unusually frequent ankle sprains.
Diagnosis
A patient is asked to step with full body weight on the symptomatic foot, keeping the unaffected foot off the ground. The patient is then instructed to "raise up on the tip toes" of the affected foot. If the posterior tibial tendon has been attenuated or ruptured, the patient will be unable to lift the heel off the floor and rise onto the toes. In less severe cases, the patient will be able to rise on the toes, but the heel will not be noted to invert as it normally does when we rise onto the toes. X-rays can be helpful but are not diagnostic of the adult acquired flatfoot. Both feet, the symptomatic and asymptomatic - will demonstrate a flatfoot deformity on x-ray. Careful observation may show a greater severity of deformity on the affected side.
Non Surgical Treatment
Treatment of plantar fasciitis is sometimes a drawn out and frustrating process. A program of rehabilitation should be undertaken with the help of someone qualified and knowledgeable about the affliction. Typically, plantar fasciitis will require at least six weeks and up to six months of conservative care to be fully remedied. Should such efforts not provide relief to the athlete, more aggressive measures including surgery may be considered. The initial goals of physical therapy should be to increase the passive flexion of the foot and improve flexibility in the foot and ankle, eventually leading to a full return to normal function. Prolonged inactivity in vigorous sports is often the price to be paid for thorough recovery. Half measures can lead to a chronic condition, in some cases severely limiting athletic ability.

Surgical Treatment
Surgery may be necessary in situations where the symptoms are likely to get worse over time, or when pain and instability cannot be corrected with external orthopedic devices. There are many types of surgical procedures, including cavus foot reconstruction, which can be performed to correct the foot and the ankle and restore function and muscle balance.
Stretching Exercises
Massage therapy is a great way to loosen muscles and help improve mobility in in your feet. As many people with foot pain have discovered, tight muscles in your legs or back can lead to tense foot muscles. All those muscles are connected, so tension in your back can cause tension in your legs which can pull the tendons in your feet and cause stiffness and pain. Getting acupuncture or a professional full body massage are probably the best ways to deal with this, but there are also some simple tricks you can do at home to help keep muscles limber. These are great for loosening up and improving circulation, both before and after exercise. Place a tennis ball under the arch of your bare foot and roll it around, stretching the muscles in your foot and promoting blood flow. You can also roll the ball under your calves and upper legs to work out stiffness and knots. If you feel the tennis ball is too easy, try a lacrosse ball for deeper massaging. This is also demonstrated in the exercise video above. Use a foam roller, those big overpriced rolls of foam that are now available in every department and sporting goods store are fantastic for self-massage (why a roll of foam costs $30 is beyond us, but they do work wonders-our advice is to not waste money on the more expensive fancy grooved ones because even the simplest rollers work great). The exercises you can do with foam rollers seem to be endless, and there are literally hundreds of free videos online showing how to use them to massage every part of your body. Here's one we picked out that specifically targets foot and leg muscles related to arches and plantar fasciitis.
Managing With A Bunion
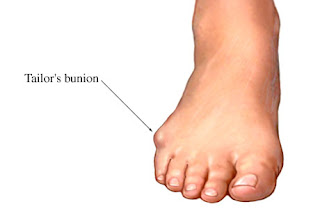
People think of a bunion as being as a bump on the side of the foot near the big toe. However, bunions go deeper than what we can see. Although the skin might be red, a bunion actually reflects a change in the anatomy of the foot. Bunions happen over time. What begins as the big toe pointing toward the second toe ends up as changes in the actual alignment of the bones in the foot. There is also a condition called tailor?s bunion or bunionette. This type of bump differs from a bunion in terms of the location. A tailor?s bunion is found near the base of the little toe on the outside of the foot.
Causes
Bunions are not inherited, but do tend to run in families. What is inherited is the poor or faulty foot type, that mechanically can lead to the instability around the joint that will eventually lead to bunions, how soon, how quickly and how bad they are or become is assumed to be very dependant on the footwear. A number of other factors are known to play a role in the cause of bunions and hallux valgus. Bunions can follow foot injuries and develop in those with neuromuscular problems. Those with flat feet or pronated feet appear to be more prone to the instability about the joint and have a higher incidence of bunions. Some activities (eg ballet dancing) puts added pressure on the joint and may increase the chance of bunions developing.
Symptoms
The most obvious symptoms of a bunion are. Pain in the area of the MTP joint, the joint where your big toe connects to your foot. Bending of the big toe in towards the other toes. An enlarged bump of bone or tissue at the MTP joint. Each symptom can range in degree from small to severe. Sometimes the pain can be sufficient to make it difficult to walk in normal shoes. Other symptoms may include. Swelling and inflammation of the skin around the MTP joint. Thickening of the skin in the area of the joint. Restricted motion in your big toe. Pressure from the inward bending of your big toe can affect your other toes, leading to corns on your smaller toes. Ingrown toenails on the smaller toes. Development of hammertoes in the other toes. Calluses on the bottom of your foot. If you have any of these symptoms, especially pain, displacement of your big toe or development of a bulge, you should consider consulting your physician. Even if you're not significantly bothered by some of these symptoms, bunions tend to continue getting bigger and more serious over time and should be taken care of before they do so.
Diagnosis
Your doctor will ask questions about your past health and carefully examine your toe and joint. Some of the questions might be: When did the bunions start? What activities or shoes make your bunions worse? Do any other joints hurt? The doctor will examine your toe and joint and check their range of motion. This is done while you are sitting and while you are standing so that the doctor can see the toe and joint at rest and while bearing weight. X-rays are often used to check for bone problems or to rule out other causes of pain and swelling. Other tests, such as blood tests or arthrocentesis (removal of fluid from a joint for testing), are sometimes done to check for other problems that can cause joint pain and swelling. These problems might include gout , rheumatoid arthritis , or joint infection.
Non Surgical Treatment
Patients with a painful bunion may benefit from four to six physical therapy treatments. Your therapist can offer ideas of shoes that have a wide toe box (mentioned earlier). The added space in this part of the shoe keeps the metatarsals from getting squeezed inside the shoe. A special pad can also be placed over the bunion. Foot orthotics may be issued to support the arch and hold the big toe in better alignment. These changes to your footwear may allow you to resume normal walking immediately, but you should probably cut back on more vigorous activities for several weeks to allow the inflammation and pain to subside. Treatments directed to the painful area help control pain and swelling. Examples include ultrasound, moist heat, and soft-tissue massage. Therapy sessions sometimes include iontophoresis, which uses a mild electrical current to push anti-inflammatory medicine to the sore area. This treatment is especially helpful for patients who can't tolerate injections.

Surgical Treatment
Most bunions can be treated without surgery. But when nonsurgical treatments are not enough, surgery can relieve your pain, correct any related foot deformity, and help you resume your normal activities. An orthopaedic surgeon can help you decide if surgery is the best option for you. Whether you've just begun exploring treatment for bunions or have already decided with your orthopaedic surgeon to have surgery, this booklet will help you understand more about this valuable procedure.
Prevention
Here are some tips to help you prevent bunions. Wear shoes that fit well. Use custom orthotic devices. Avoid shoes with small toe boxes and high heels. Exercise daily to keep the muscles of your feet and legs strong and healthy. Follow your doctor?s treatment and recovery instructions thoroughly. Unfortunately, if you suffer from bunions due to genetics, there may be nothing you can do to prevent them from occurring. Talk with your doctor about additional prevention steps you can take, especially if you are prone to them.